What is the maximum BMI for weight loss surgery?
Significance of BMI for Weight Loss Surgery Amidst Rising Obesity Rates
Understanding the Body Mass Index (BMI) for weight loss surgery is paramount. BMI, a numerical value derived from weight and height, is a pivotal tool for evaluating a patient’s suitability for weight loss surgery. It provides a standardized measure that helps medical professionals assess the level of obesity, which is crucial in deciding the most appropriate course of action.
As we venture into the 21st century, a concerning trend looms over our global health landscape. The prevalence of obesity has reached alarming proportions, becoming a pandemic of its own. This epidemic carries a heavy burden of health implications, impacting individuals and entire healthcare systems. Obesity is intricately linked to various chronic diseases, including diabetes, cardiovascular issues, and certain cancers, contributing to increased mortality rates and soaring healthcare costs.
What is BMI?
Body Mass Index (BMI) is fundamental to weight loss surgery. It’s a numerical value derived from a person’s weight and height. Calculating BMI is a simple equation: weight in kilograms divided by height in meters squared. This formula provides a quick assessment of an individual’s body composition.
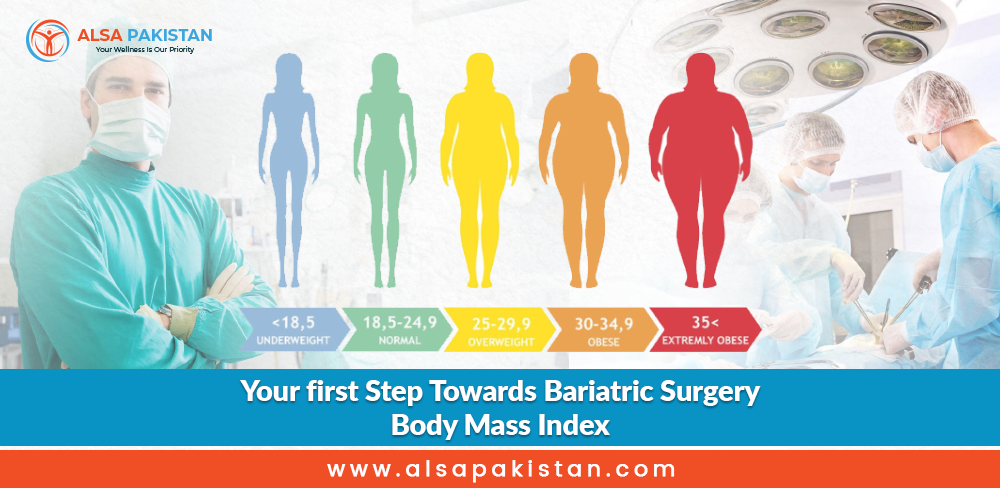
Categories of BMI and their significance
The categories of a BMI calculator are well-defined. They range from underweight to severely obese. Each category has specific implications for health. For instance, a BMI of 18.5 or less is considered underweight, while a BMI of 30 or higher signifies obesity. These categories help healthcare providers gauge the severity of a patient’s condition.
The role of BMI in assessing candidacy for weight loss surgery
When it comes to weight loss surgery, BMI plays a pivotal role. It’s a primary criterion for assessing whether someone is a suitable candidate. Generally, individuals with a BMI of 40 or higher are considered prime candidates. However, surgery might still be an option for those with a lower BMI but significant obesity-related health issues.
However, it’s crucial to acknowledge that BMI has limitations. It doesn’t account for variations in muscle mass, bone density, or factors like age and sex. Therefore, clinical judgment should accompany BMI assessments when deciding on weight loss surgery. While the BMI calculator for women and men is a valuable tool, it’s not the sole factor in determining eligibility.
Weight Loss Surgery Options
Gastric Bypass
Gastric bypass surgery is typically recommended for individuals with a BMI of 35 or more, especially if they have obesity-related health issues, such as type 2 diabetes, sleep apnea, or hypertension. It is particularly effective for patients with severe obesity, often leading to significant weight loss.
Higher BMIs are associated with more substantial weight loss after gastric bypass. Additionally, individuals with a higher BMI who undergo gastric bypass may experience significant improvements in obesity-related health conditions post-surgery.
Sleeve Gastrectomy
Sleeve gastrectomy is suitable for individuals with a BMI of 30 or higher, mainly if they prefer a less invasive option. It is also recommended for patients with obesity-related co-morbidities. It offers effective weight loss for those with moderate to severe obesity while maintaining a more straightforward surgical approach than other procedures.
Higher BMIs can lead to more pronounced weight loss with sleeve gastrectomy. However, individual factors that affects BMI and adherence to post-surgery guidelines are crucial in determining outcomes.
Roux-Y Gastric Bypass (RYGB)
RYGB is ideal for individuals with severe obesity, usually with a BMI of 40 or higher, and those who require significant weight loss. This procedure is suited for patients with severe obesity due to its ability to induce substantial weight loss and address co-morbidities. Roux-Y Gastric Bypass (RYGB) can lead to significant weight loss, especially in patients with higher BMIs, and may result in marked improvements in obesity-related health conditions.
Mini Gastric Bypass Surgery
Mini gastric bypass surgery is similar to RYGB but offers a quicker and less complex procedure, often suitable for patients with a BMI of 30 or more. It provides an alternative for individuals with moderate obesity or who prefer less invasive surgery. Patients with higher BMIs undergoing mini gastric bypass surgery may experience substantial weight loss, and improvements in co-morbidities are possible.
Single Anastomosis Duode-ileal Bypass (SADI) Surgery
SADI surgery is recommended for individuals with a BMI of 35 or higher, especially when other surgeries are unsuitable. It is an option for individuals with severe obesity or those for whom other surgeries may not be feasible. Patients with higher BMIs may achieve significant weight loss and improve obesity-related health conditions after SADI surgery.
The Role of BMI in Surgical Eligibility
Regarding bariatric surgery, Body Mass Index (BMI) is a critical determinant for eligibility. Let’s delve into its multifaceted role.
Current BMI Guidelines for Bariatric Surgery
Present guidelines generally suggest a BMI of 40 or higher for bariatric surgery or a BMI of 35 with significant obesity-related health conditions. These benchmarks have been established based on extensive research and clinical experience.
Varying Criteria Across Surgical Centers and Countries
Recognizing that BMI criteria can differ among surgical centers and even countries is essential. Local healthcare norms and available resources influence these variations. While some may adhere strictly to established guidelines, others might consider individualized factors.
Exceptions and Considerations for Patients with Exceptionally High BMIs
Patients with exceptionally high BMIs (50 or above) may face unique challenges. Sometimes, healthcare professionals may need preliminary weight loss methods or medical interventions to prepare patients for surgery. Individual health assessments play a pivotal role in deciding the most appropriate approach.
Risks and Benefits Associated with Surgery at Higher BMIs
Bariatric surgery at higher BMIs offers significant weight loss potential and improved health outcomes. However, it’s not without risks. A higher BMI can be associated with an increased risk of surgical complications, longer hospital stays, and an extended recovery. Healthcare professionals must carefully weigh the benefits against these potential drawbacks.
Factors that affect weight loss surgery beyond BMI
While BMI is crucial in assessing eligibility for weight loss surgery, other factors beyond body mass index are equally important. These considerations provide a more comprehensive picture of a patient’s suitability for surgery.
The Importance of Assessing Overall Health and Medical History
Beyond BMI, a comprehensive assessment of overall health is vital. Pre-existing medical conditions, such as heart disease, sleep apnea, or diabetes, can impact surgical candidacy. A thorough evaluation helps identify potential risks and determine the best approach.
Co-morbidities and Their Impact on Surgical Candidacy
Co-morbidities, or concurrent health conditions, often accompany obesity. These conditions, like hypertension or high cholesterol, can influence the decision to undergo surgery. Some patients with lower BMIs may still be candidates if they have severe co-morbidities, highlighting the need for a holistic approach.
Psychological Evaluations and Their Significance in the Selection Process
Mental health is a critical component of surgical readiness. Psychological evaluations assess a patient’s emotional well-being, understanding of the surgical process, and commitment to post-operative lifestyle changes. These evaluations help ensure that healthcare professionals prepare patients for the psychological challenges that may arise post-surgery.
Weight Loss Surgery Outcomes at Different BMIs
The impact of weight loss surgery can vary significantly based on an individual’s BMI. Understanding these variations is essential in setting realistic expectations and evaluating potential benefits and risks.
Expected Weight Loss Outcomes Based on BMI
The amount of weight loss achieved through surgery correlates with the initial BMI. Higher BMIs tend to result in more significant weight loss. For instance, individuals with BMIs above 40 often experience substantial reductions in excess body weight.
The Potential for Improvements in Obesity-Related Health Conditions
Weight loss surgery isn’t solely about shedding pounds. It can also lead to remarkable improvements in obesity-related health conditions. Conditions like type 2 diabetes, sleep apnea, and hypertension often show marked improvement or remission, especially in individuals with higher BMIs.
Long-Term Success and Complications Associated with Higher BMIs
BMI can influence long-term success after weight loss surgery. Patients with higher initial BMIs may face more challenges in maintaining weight loss over time. Furthermore, higher BMIs increase the risk of surgical complications, including wound infections and leaks, which healthcare professionals must carefully manage.
BMI for Weight Loss Surgery: Your Key to Transformation
We cannot overstate the significance of BMI in the decision regarding weight loss surgery. It serves as a guiding light, helping patients and healthcare professionals navigate the complex landscape of bariatric procedures.
BMI, a simple yet powerful metric, remains a cornerstone in assessing eligibility for weight loss surgery. It helps identify candidates and provides insights into the potential outcomes, both in terms of weight loss and improvements in obesity-related health conditions. However, BMI is not the sole determinant; healthcare professionals should consider individual health, preferences, and other factors alongside BMI.
In pursuing a healthier and more fulfilling life, remember that BMI is a valuable tool but not the only one. The journey towards weight loss surgery is deeply personal and requires a holistic approach. By working closely with healthcare professionals, you can chart a path that aligns with your unique needs and aspirations, ensuring the best possible outcomes in your weight loss journey.